
If Lower Limb Swelling Occurs, Beware of Deep Vein Thrombosis! Understand the Symptoms, Causes and Treatment of Venous Thrombosis At Once
Office workers often sit for long periods of time due to their busy work schedule, but sitting still for long periods of time may lead to poor blood circulation in the long run, and in severe cases, may even cause blood clots! Cases have shown that long-term sitting or taking contraceptive pills can lead to gradual swelling, pitting edema and even skin ulcers in the lower limbs, which may be deep vein thrombosis (DVT).
What exactly is deep vein thrombosis, and what effects and harms does it have on the body? We provide readers with further information on the causes, prevention, and treatment of deep vein thrombosis.

What is deep vein thrombosis?
Deep vein thrombosis occurs when a blood clot or thrombus forms in one or more deep veins in the body. The symptoms may occur in the arms, legs, or other parts of the body; in most people, they occur in the legs, causing pain or swelling in the lower limbs, or they may not cause any symptoms.
However, it is important to note that deep vein thrombosis does not only affect the legs. Blood clots in the veins may break up and travel along the blood flow into the lungs, thereby blocking the blood flow in the lungs and causing pulmonary embolism (PE). ), severe cases may be life-threatening. Deep vein thrombosis and pulmonary embolism are collectively called venous thromboembolism (VTE), and they are also one of the most commonly discussed conditions when thrombosis occurs.
Lower extremity venous thrombosis symptoms
Some patients with deep vein thrombosis will not experience any discomfort, while others may experience the following symptoms:
- Swelling in one leg, less often both legs together
- A pain that usually starts in the calf and feels like a cramp or soreness
- The skin on the legs changes color or turns red
- A hot feeling in the legs
When should you seek medical attention for venous thrombosis of the lower extremities?
When you find that you have the above suspected symptoms of deep vein thrombosis, do not ignore it and go to the hospital for examination as soon as possible. Especially if you experience severe discomfort due to pulmonary embolism, you must seek medical attention immediately. Possible symptoms of pulmonary embolism are as follows:
- Sudden shortness of breath
- Feeling chest pain or discomfort when taking deep breaths or coughing
- Feeling like you have a headache, dizziness, or fainting
- Rapid pulse
- Coughing up blood
Causes and high-risk groups of deep vein thrombosis
According to Virchow triad, the causes of deep vein thrombosis can be divided into the following three major mechanisms:
- Blood vessel injury
- Stagnation of blood
- Hypercoagulable state
According to the latest “European Society of Cardiology ESC Guidelines” in 2020, the risk level of deep vein thrombosis can be subdivided into the following three categories:
- High risk
- Lower limb fracture
- Hospitalization for heart failure or atrial fibrillation (within the first 3 months)
- Hip or knee replacement surgeryMajor trauma
- Myocardial infarction (within the first 3 months)
- People who have suffered from deep vein thrombosis
spinal injury
- Medium risk
- Chemotherapy
- Congestive heart failure or respiratory failure
- Oral contraceptive pills
- Hormone replacement therapy
- Infections: especially pneumonia, urinary tract infections, human immunodeficiency virus (HIV)
- Inflammatory bowel disease
- Cancer (most commonly metastatic cancer)Thrombophilia: such as hereditary thrombophilia
- Low risk
- Bedridden: for more than 3 days
- Prolonged sitting: such as airplane economy class syndrome, riding in a car or working
- Diabetes, hypertension
- Old age
- Obesity
- Pregnant
- Varicose veins
Complications of deep vein thrombosis
- Pulmonary embolism: Pulmonary embolism accounts for one-third of symptomatic venous thromboembolism (VTE). Once you suffer from pulmonary embolism, the mortality rate is very high, higher than the mortality rate from acute coronary syndrome (ACS).
- Post-thrombotic syndrome (PTS) refers to the clinical symptoms manifested by long-term comorbidities after deep vein thrombosis (DVT). This includes pain, itching, swelling, heaviness, varicose veins in the affected leg, brown or red discoloration of the skin, and even ulcers.
How do you know if you have deep vein thrombosis?
Doctors can observe whether there is swelling, discoloration or tenderness in the affected area through consultation and physical examination. In addition, doctors may use the following methods for further diagnosis:
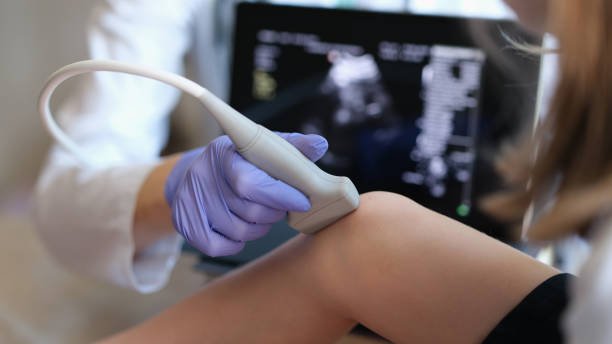
- Ultrasound: Ultrasound waves can penetrate tissue, reflect back and display images through machine calculations to determine the location of the embolism. However, because newly formed thrombi are soft, they are not easily detected under ultrasound. Therefore, the diagnosis of deep vein thrombosis must use compression ultrasound (Compression ultrasound) method. Under normal circumstances, veins will collapse with gentle pressure, but if a blood clot is present, the vein will not collapse.
- Blood test: D-dimer has a high negative predictive value. If the D-dimer value in the blood is found to increase, it means that the patient may have venous thrombosis or pulmonary embolism. If D-dimer is normal, the possibility of venous thrombosis can almost be ruled out, because the incorrect diagnosis rate is only 1%.
- Venography/phlebography: A catheter is inserted from the groin into the femoral artery, an iodine-containing contrast agent is injected into the blood vessel, and X-rays are used to find the location of the venous embolism.
- Computed tomography (CT scan): It can take X-ray pictures from more sections and is mainly used to diagnose pulmonary embolism.
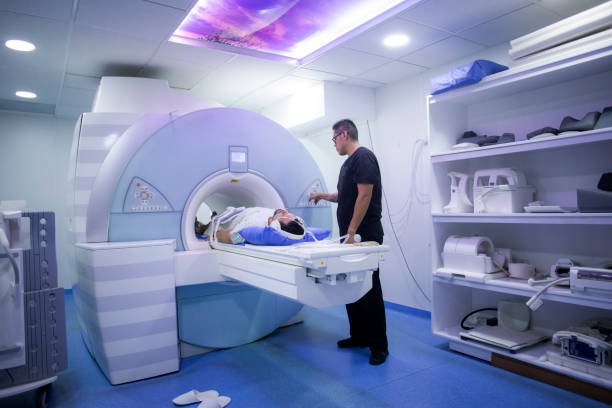
- Magnetic resonance scan (MRI): uses radiofrequency and magnetic fields to construct images. Since there is no concern about radiation, it is suitable for pregnant women as an option for examination.

Treatment of deep vein thrombosis
The treatment of deep vein thrombosis focuses on preventing the thrombus from expanding and rupturing, and preventing the risk of future thrombus formation. The treatment methods are divided into the following categories:
- Use anticoagulants: reduce the blood’s ability to clot to prevent thrombosis. For example, heparin, low molecular weight heparin, warfarin, and Novel Oral Anticoagulant drugs (NOAC). Overall, the new anticoagulants are almost as effective as warfarin and can reduce the risk of bleeding. It is easy to use and the efficacy is not affected by food.
- Thrombolytics: For example, tPA (tissue plasminogen activator) activates plasminogen into plasmin, thereby dissolving fibrin. This process of dissolving fibers is called fibrinolysis.
- Elastic stockings: Give pressure to the legs, enhance blood circulation, improve leg varicose veins and prevent blood clots.
- Inferior vena cava filter (IVC filter): To prevent blood clots from breaking off and flowing to the lungs to cause pulmonary embolism, doctors may place a filter in the inferior vena cava. When the patient is not suitable for the use of anticoagulants, or when anticoagulants are used and the patient still suffers from recurrent attacks, an inferior vena cava filter is suitable.
- Thrombus removal surgery: using methods such as resection, extraction or shock waves, combined with thrombolytic agents to remove thrombus
How to prevent deep vein thrombosis
The formation of venous thrombosis can be effectively prevented through the following methods:
- Avoid sitting or lying down for a long time: you should get up and move around for a few minutes every once in a while, and you should not cross your legs when sitting for a long time.
- When the environment requires you to sit for a long time and it is inconvenient to stand up and move (such as flying), please try to moderately stretch and contract your leg muscles and limbs.
- Quit smoking
- Regular exercise
- Avoid wearing tight clothing
- Maintain a standard weight
- Drink more water
Warning for Pregnant Women
Pregnant women are also at high risk for deep vein thrombosis. Considering the health status of the mother and fetus, it is advisable to use D-dimer, compression ultrasound, MRI and other testing methods during diagnosis to avoid negative effects on the fetus. In addition, heparin and warfarin carry the risk of teratogenesis and are not suitable as treatments during pregnancy.












