
Valvular Heart Disease
There are many types of heart disease. In addition to the common hypertensive heart disease and coronary heart disease, valvular heart disease also troubles many people. Heart problems, this article will take you to understand the function and abnormal symptoms of valves, as well as how to treat and prevent valvular heart disease.
What is valvular heart disease?
There are 4 valves with different positions in our heart, which are responsible for controlling the passage of blood and preventing blood from flowing back. The names of these 4 valves are:
- Aortic valve:
located between the left ventricle and the aorta - Pulmonary valve:
located between the right ventricle and the pulmonary artery - Tricuspid valve (Tricuspid):
located between the right atrium and right ventricle - Mitral valve (Mitral):
located between the left atrium and left ventricle
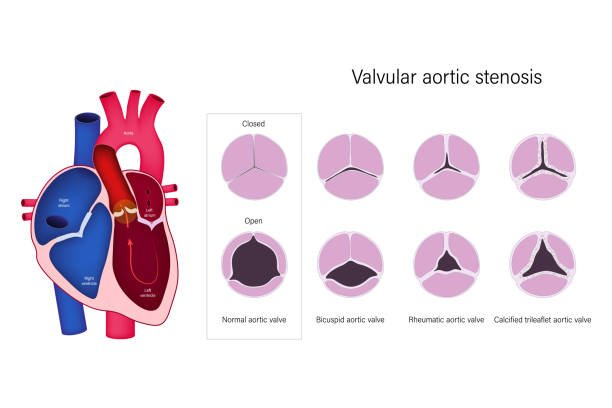
Generally speaking, the aortic valve and mitral valve are more likely to cause valvular heart disease, because these two parts are the only way for the heart to pump out oxygenated blood for systemic circulation. When the blood pressure and blood flow rate are fast, situation, it is more likely to be damaged. When a valve becomes narrow or stiff and cannot fully close or open, it can cause valve prolapse or valve stenosis.
- Valve prolapse:
The valve cannot seal completely, and severe atresia may cause blood to flow back into the ventricle or atrium. - Valvular stenosis:
Narrow valves open very narrow channels, making the heart work harder to pump blood out.
There are many possible causes of valvular heart disease, such as congenital structural abnormalities, or acquired factors, such as infection with rheumatic fever (Rheumatic fever), infective endocarditis (Infective endocarditis) or aging, etc., which will be further introduced later in this article.
Symptoms of valvular heart disease
The symptoms that may appear vary from person to person, and some people may not even have symptoms until they are diagnosed if they have been suffering from the disease for many years. The following are common symptoms of valvular heart disease:
- Angina pectoris
- heart murmur
- abdominal bloating
- fatigue
- Dizziness
- faint
- Difficulty breathing, rapid breathing
- swelling of the legs or ankles
- arrhythmia
Diagnostic methods for valvular heart disease
The doctor may first use a stethoscope to check if there is a murmur in your heart. If the blood flow is blocked or the valves are abnormal, a heart murmur may occur. The following are other diagnostic methods for valvular heart disease:
- Electrocardiography (ECG or EKG for short):
By attaching electrode patches to the heart, legs, arms, etc., an electrocardiogram instrument is used to detect the potential changes in the heart, and the results are displayed on the screen. - Echocardiography:
Uses ultrasound to observe heart activity, and can also take and record heart images. - Chest X-ray:
This can look for an enlarged heart, which can lead to some types of valvular heart disease. - Cardiac MRI:
Uses magnetic fields and radio waves to create detailed images of the heart for easy viewing. - Exercise stress test:
Use exercise equipment such as a treadmill or stepper to observe the blood circulation and delivery when the heart is exercising. - Coronary angiography:
Commonly known as cardiac catheterization, it is mainly used for coronary artery examination, but can also be used as an auxiliary examination for other heart diseases. A thin tube is inserted through the groin or arm and a dye is injected into the blood vessels so that X-ray equipment can be used to observe blood flow in the coronary arteries.
Risk of valvular heart disease
60% of valvular heart disease is caused by rheumatic heart disease. The following are common causes of valvular heart disease:
- Congenital valve defects:
Congenital abnormalities in the size or shape of the valves will increase the incidence of valvular heart disease. For example, the aortic valve normally has three leaflets, but some people with only two leaflets are prone to atresia. situation. - Marfan syndrome:
a hereditary connective tissue disease that easily causes heart valve abnormalities. - Rheumatic fever:
usually caused by an infection caused by Streptococcal bacteria, such as strep throat (Laryngopharyngitis). Rheumatic fever itself does not infect the heart, but the antibodies and inflammatory substances produced by the body can inflame and scar the heart valves, leading to valve stenosis or prolapse, leading to rheumatic heart disease. - Infectious endocarditis:
Also known as bacterial endocarditis, if bacteria enter the blood and adhere to the heart valves along the blood flow, they may cause holes or scabs in the valves, destroying valve function. - Radiation therapy:
Some cancer patients may need radiation therapy to the chest, which may increase the risk of valvular heart disease. - Elderly:
The older you are, the easier it is for the valves to affect their function due to aging. Years of blood erosion will make the valves thicker and harder, increasing the chance of suffering from valvular heart disease. - People with high cholesterol:
High blood cholesterol levels may increase the chance of valve calcification, leading to valve stenosis, but not all cholesterol is bad. For example, low-density lipoprotein (LDL, commonly known as bad cholesterol) will increase the risk of sclerosis, but high-density lipoprotein (LDL, commonly known as bad cholesterol) will increase the risk of sclerosis. HDL (commonly known as good cholesterol) actually helps prevent plaque buildup. - Women:
Women are more likely than men to suffer from rheumatic fever and develop valvular heart disease.
Complications of valvular heart disease
Valvular dysfunction may result in the following complications:
- Heart failure:
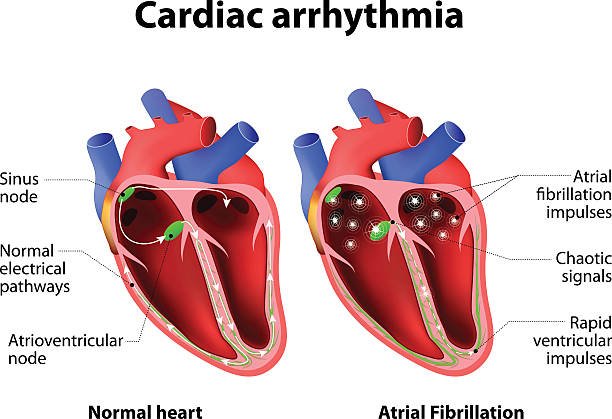
Certain areas of the heart weaken due to a lack of blood, or the heart cannot pump enough blood throughout the body. - Arrhythmia:
Blocked blood flow to the heart affects the electrical activity of the heart, resulting in abnormal heart rate. - Stroke:
Blockage or rupture of blood vessels in the brain, resulting in loss of body functions. - Cardiac hypertrophy:
Whether a narrow valve forces the heart to increase its pulsating force, or valve insufficiency causes blood to flow backward, causing the ventricles to fill with blood and expand, this can easily lead to cardiac hypertrophy. Severe cardiac enlargement may turn into heart failure.
Treatment of valvular heart disease
1.Medication
Minor valve problems may require continued monitoring, but other symptoms caused by the valves can be treated with medications.
- Diuretic:
can reduce edema and lower blood pressure. - Anticoagulant:
Prolongs blood clotting time and reduces the chance of heart valve thrombosis. - Antiarrhythmics:
such as Calcium channel blockers (CCB) and beta-blockers (β-Blocker), can improve arrhythmias. - Angiotensin converting enzyme inhibitors (ACEI):
The main function is to inhibit the conversion of angiotensin I to angiotensin II to prevent it from increasing blood pressure; the other function is to prevent angiotensin from catalyzing Delays the hydrolysis of Bradykinin to promote vasodilation. Can be used to improve conditions such as high blood pressure and heart failure. - Beta-blocker (β-Blocker):
can reduce heart rate and blood pressure, reducing the burden on the heart. If the patient has had a heart attack before, taking beta-blockers can help reduce the chance of another myocardial infarction in the future. - Vasodilator:
helps the smooth muscles around blood vessels relax, dilates blood vessels, lowers blood pressure, promotes blood flow, and improves blood reflux caused by valve insufficiency.
If the valve is severely damaged or loses function, it will need to be repaired through the following surgeries or replaced with an artificial or biological valve:
2.Valve repair:
If the valve damage is not serious, repair is usually the main method.
3.Thoracotomy:
Depending on the condition of the valve, different repair methods will be selected. If the valve is incompletely atretic, the doctor may sew the bottom ring of the valve or install an artificial ring at the base of the valve so that the valve can be completely closed; if the valve is stenotic, the doctor may Consider cutting the valve leaflets to improve blood obstruction.
- Percutaneous coronary intervention (PCI): Also known as balloon angioplasty, the advantage is that it does not require an incision in the chest to operate. The doctor will insert a thin catheter from the groin or arm, through the blood vessels to the heart, and inflate the balloon at the end of the catheter to expand the narrowed valve and improve blood flow; if the valve is incompetent, the balloon will be replaced with a valve The clip is delivered to the side of the valve in the same way, so that the clip is fixed to clamp the valve leaflets and prevent blood from flowing back.
- Transcatheter aortic valve implantation (TAVI): also called Transcatheter aortic valve replacement (TAVR). Traditional valve replacement requires thoracotomy, but the advantage of minimally invasive surgery like TAVI is that the patient’s postoperative recovery period is shorter and the scars produced are smaller. In fact, its concept is somewhat similar to the balloon dilatation mentioned above. It only requires a small incision in the groin or chest, and a catheter carrying an artificial valve can be inserted and guided to the heart for valve replacement.
4.Replacement valve:
If the valve is severely damaged, valve replacement may be considered to maintain valve function. Artificial valves are mainly divided into mechanical valves and biological valves. The following are the advantages, disadvantages and applicable objects of the two.
- Mechanical valve: The earliest artificial valve, made of metal, ceramic or plastic. Its advantages are long service life and low cost, but the use of mechanical valves requires lifelong use of anticoagulants to reduce the formation of blood clots and avoid thrombosis, so it is more suitable for young people or people who are not taking anticoagulant drugs.
- Biological valves: Most are made of cow or pig tissue. They are easier for the human body to adapt to than mechanical valves, so they are less likely to produce blood clots. Of course, it would be better to accept human heart valve transplants, but the vast majority are still based on animal tissue products. Biological valves are expensive and less durable, but have a lower chance of thrombosis. They are suitable for the elderly or patients with other serious diseases. Moreover, users only need to take anticoagulants for a short period of time after surgery. They are suitable for those who plan to become pregnant. People choose because taking anticoagulants can have adverse effects on pregnancy and the fetus.
Preventive methods for valvular heart disease
Although valvular heart disease is mostly caused by congenital defects or rheumatic fever, damage to the heart caused by an unhealthy lifestyle and normal aging may cause valvular disease. Here are 6 ways to prevent valvular heart disease:
- Regular follow-up:
Through examination, it is usually possible to know whether the heart valves have congenital defects or poor function. The condition may not necessarily be bad enough to require surgical treatment. Continuous follow-up and improvement of daily life can reduce the threat of valvular heart disease. - Healthy diet:
Adopt a low-oil, low-sugar, low-salt and high-fiber diet to reduce blood lipid accumulation and reduce the chance of obesity. - Oral health:
People with periodontal disease may bleed frequently when brushing their teeth, which allows bacteria to invade the body and increase the chance of infective endocarditis. - Moderate exercise:
For people with congenital valvular stenosis, it is recommended to discuss the time and type of exercise with a doctor, and avoid overly intense exercise to avoid causing heart discomfort. - Quit smoking:
Smoking can damage blood vessels and increase the risk of atherosclerosis; the nicotine in cigarettes can also increase blood pressure; the emitted carbon monoxide can reduce the oxygen-carrying capacity of the blood. - Avoid alcohol abuse:
Excessive alcohol consumption can cause blood pressure and triglycerides (Triglycerides). Triglycerides are a type of fat in the blood. Excessive levels of triglycerides may increase the risk of atherosclerosis. - Check your cholesterol:
You should have your cholesterol checked at least every 5 years after age 20. Most people’s LDL levels should be below 130 mg/L or below 3.4 mmol/L. If you are at high risk for heart disease, your LDL level may need to be kept below 100 mg/L or 2.6 mmol/L.












