7 Major Symptoms of Pancreatic Cancer! “King of Cancer” Pancreatic Cancer Causes, Survival Rate, and Treatment
Pancreatic cancer is almost asymptomatic in its early stages, but once it develops, it metastasizes quickly and has a low cure rate. Only 20% of patients survive. Therefore, it is also called the “King of Cancer.” Many celebrities, such as Apple founder Steve Jobs, etc., have suffered from pancreatic cancer. Passed away one after another due to pancreatic cancer; what is the survival rate of pancreatic cancer? Can it be diagnosed and treated at an early stage? This article will introduce the causes, symptoms, diagnosis and treatment of pancreatic cancer one by one.
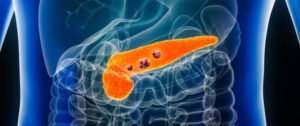
Where is the pancreas located? What is the function?
The pancreas, also known as the pancreas, is an organ located in the retroperitoneal cavity. In addition to the well-known secretion of insulin and glucagon, which is responsible for regulating the concentration of glucose in the blood, its main function is to secrete pancreatic juice. Pancreatic juice contains protease, amylase, etc., which are important enzymes that are indispensable for human digestion.
What causes pancreatic cancer? Why is it so hard to find?
The cause of the pancreas, like many cancers, has no standard answer, but many reports and studies now show that diabetes, smoking, alcoholism, obesity, etc. are regarded as one of the risk factors for pancreatic cancer. Pancreatic cancer occurs when pancreatic cells become cancerous, and 92% of them are adenocarcinoma. However, the main reasons for its high mortality rate can be summarized into the following two points:
- Location: The retroperitoneal cavity where the pancreas is located is located on the back side of the spine. It can be said to be a quite secretive location. This also makes it difficult to detect cancerous lesions in the pancreas early.
- Symptoms are not obvious: Pancreatic cancer has almost no symptoms in the early stage, causing many patients to feel uncomfortable. Only when they go to the hospital for examination do they discover that the condition is quite serious.
7 warning signs of pancreatic cancer
When symptoms of pancreatic cancer appear, it usually means that the tumor has grown to a certain size. If you find that you have the following symptoms that may appear to be pancreatic cancer, please be sure to go to the hospital for examination as soon as possible to avoid delaying treatment:
- Jaundice
Jaundice is the most common symptom among pancreatic cancer patients. An enlarged malignant tumor may compress the common bile duct, preventing bile secreted by the liver from entering the small intestine to break down bilirubin, leading to jaundice.
The patient’s skin and the whites of the eyes will turn yellow, the urine will be brown, the stool will be gray or white, or the fat will float on the water because fat cannot be broken down. In addition, the patient may also have itchy skin. - Abdominal or back pain
An enlarged pancreatic tumor may press on other organs or surrounding nerves, causing back or abdominal pain. These symptoms usually progress slowly, causing abdominal pain for more than six months, and are exacerbated when lying down or extending the spine. - Abnormal weight loss
Loss of appetite and indigestion may lead to weight loss in patients with pancreatic cancer. - Feel sick and vomit
If the tumor compresses the stomach, the patient may experience nausea and vomiting, which may also lead to weight loss and a reduced desire to eat. - Gallbladder and liver enlargement
When a tumor compresses the common bile duct, bile that cannot be transported out may accumulate in the gallbladder, causing the gallbladder to become enlarged. If the tumor spreads to the liver, hepatomegaly may occur. - Diabetes
Although rare, pancreatic cancer may disrupt insulin production, leading to diabetes - Thrombus
In some cases, people with pancreatic cancer may develop deep vein thrombosis. The patient’s lower legs may be swollen and painful. If the blood clot breaks off and remains in the lungs, it may cause pulmonary embolism.

High-risk groups for pancreatic cancer
People who meet the following conditions have a higher chance of developing pancreatic cancer:
- Older age: Pancreatic cancer is more likely to occur in the elderly, with most patients over 60 years old.
- Family history of pancreatic cancer: When a relative or family member has pancreatic cancer, your risk of developing the disease is also higher than the average person.
- Gene mutations: People with PRSS1, SPINK1, CFTR, Chymotrypsin C (CTRC) gene mutations may have a higher chance of developing pancreatitis or pancreatic cancer. Among them, people with PRSS1 and SPINK1 gene mutations are 50 to 80 times more likely to develop cancer than the average person, and they belong to an ultra-high risk group for pancreatic cancer.
It is worth mentioning that other genetic mutations such as BRCA1, BRCA2, CDKN2A, MLH1, ATM, and TP53 are associated with pancreatic cancer, but they are also associated with other diseases. For example, BRCA1 and BRCA2 mutations are key risk factors for breast and ovarian cancer.
- Other genetic diseases: such as Peutz-Jeghers syndrome (PJS) or Lynch syndrome (HNPCC)
- Pancreatic inflammation: It was mentioned earlier that some mutated genes can cause hereditary pancreatitis. However, even if it is not related to genetics, people with pancreatic inflammation still need to be careful because they have a higher chance of developing pancreatic cancer.
- Smoking, alcoholism, and an addiction to processed meat may lead to chronic diseases and increase the risk of cancer.
How pancreatic cancer is diagnosed
In most cases, health examinations are not suitable for preventing pancreatic cancer, because routine examinations rarely specifically target the pancreas, which is one of the reasons why pancreatic cancer is not easy to detect in its early stages.
The main screening methods for pancreatic cancer are as follows:
- Tumor markers: Also known as tumor index, there are two main types: CEA and CA 19-9, but they are not very accurate in terms of examination accuracy. This is because patients may also have increased tumor index due to other diseases.
- Computed tomography (CT scan): Provides cross-sectional images, mainly used to check whether pancreatic cancer has spread to surrounding organs.
- Magnetic resonance scan (MRI): suitable for observing the presence of lesions in the pancreatic duct and bile duct, and can also be performed together with angiography.
- Ultrasound examination: Since abdominal pain is one of the common symptoms of pancreatic cancer, if the patient has abdominal pain, abdominal ultrasound is usually used for preliminary examination. If pancreatic cancer is suspected, other imaging such as CT or MRI may be performed. examine.
- Angiography (Angiography): By injecting a developing agent into the blood vessels, and then using X-rays to see whether the blood flow in a specific area is blocked or has abnormal growth (which may be new blood vessels to supply tumors).
- Endoscopic retrograde cholangiopancreatography (ERCP): An endoscope is inserted through the throat until the endoscope reaches the anterior part of the small intestine to confirm whether the bile duct and pancreatic duct are blocked. This examination can also collect tumor tissue for biopsy.
- Biopsy: Take a part of the tumor tissue and observe it through a microscope to make further judgments (pancreatic cancer staging or subsequent course of treatment).
What are the treatments for pancreatic cancer?
The treatment of pancreatic cancer depends on the situation. If the tumor can be removed, surgery is generally given priority. If the tumor is in the head of the pancreas or has spread to the duodenum, the tumor may be removed using a Whipple operation (also known as duodenectomy); if the tumor is in the body or tail of the pancreas , distal pancreatectomy may be used.
Pancreatic cancer survival rates?
As mentioned earlier, pancreatic cancer is difficult to detect in its early stages, especially tumors outside the head of the pancreas. Obvious symptoms will not appear until a very late stage due to compression or spread. Therefore, many patients may have reached the final stage of pancreatic cancer after diagnosis.
Pancreatic cancer has a high mortality rate of more than 80%. This may be because up to 90% of pancreatic cancer patients cannot be eradicated through surgery, resulting in a 5-year survival rate of less than 5%.
Although total pancreatectomy is available, this operation can easily damage the endocrine and exocrine functions, so total pancreatectomy is usually not performed.
For patients with terminal pancreatic cancer whose tumors are too large to be eradicated, doctors may use radiotherapy and chemotherapy to alleviate the patient’s discomfort and prolong life, or perform gastric bypass surgery to drain accumulated bile into the small intestine to improve the life of terminal patients. quality.
How to prevent pancreatic cancer?
Since the causes of most cancers are unknown, it is recommended that everyone adopt healthy lifestyle habits such as quitting smoking, drinking less alcohol, avoiding exposure to chemicals, eating healthily, and exercising regularly to reduce the risk factors that induce cancer. However, the tricky thing about pancreatic cancer is that there are almost no symptoms in the early stage, and the examination is very cumbersome and the incidence rate is low. Therefore, it is recommended that high-risk groups with a family history of pancreatic cancer or genetic mutations should arrange regular examinations at the same time to ensure Advantages of early detection and early treatment.
For ordinary people, it is recommended that maintaining good living habits should be the priority, which is far more practical than regular check-ups. At the same time, they should always pay attention to their physical changes. If they feel unwell, they may wish to go to the hospital for check-up as soon as possible.